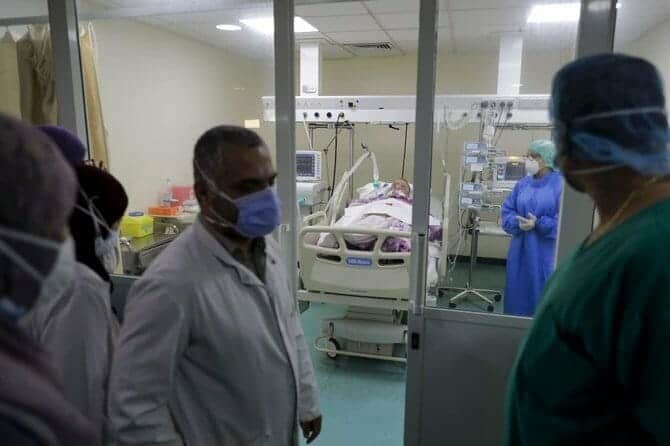
By and large, Middle East governments acted quickly to control the spread of Covid-19 when the pandemic erupted. But gradually, the strain on the health systems of Arab countries began to manifest differently, like elsewhere in the world.
The better-equipped and better-prepared rich Gulf countries, which focused on the medical side of the response, escaped its devastating effects than their poorer cousins such as Lebanon, Tunisia, and Jordan.
‘Catastrophic’ situation in Tunisia
Tunisia is currently experiencing the most severe Covid-19 crisis in North Africa. The country’s healthcare system is “collapsing” amid a wave of Covid-19 infections in recent weeks, resulting in a “catastrophic” situation, according to the health ministry. On July 8, 2021, Tunisia recorded 9,823 cases of Covid-19 and 134 deaths from the virus, the highest daily toll since the pandemic began in early 2020.
Only 4 percent of Tunisians have received complete vaccination, causing the most contagious Delta variant to spread across the country.
The expansion of the Corona outbreak in Tunisia and the disastrous situation that it has reached comes when the country is in the middle of a violent tug-of-war between the political parties.
Since the outbreak of the pandemic last year, Tunisian activists have frequently referred to the deteriorating state of the health sector’s infrastructure, as well as the authorities’ failure to take the issue of providing vaccines to people seriously. It is estimated that only about half a million Tunisians have received two doses of the Corona vaccine so far in a country of 20 million.
Port blast, failing economy worsen Lebanon’s healthcare woes
Lebanon has been in the middle of the worst economic, health, and social crisis in decades since late 2019. The pandemic, and the huge explosion in Beirut’s port in August 2020, aggravated Lebanon’s already difficult situation. The weak public health system, which was already struggling from frequent shortages of medicines and other medical supplies, was further harmed.
Lebanon is one of the most challenging countries globally to deal with the pandemic and vaccination efforts, and it requires additional support. The port explosion also destroyed infrastructure, including several hospitals, besides killing hundreds and injuring thousands. Furthermore, the Health ministry’s central warehouse, which stored all the country’s medical supplies, was severely damaged.
The government’s failure to pay dues to be public and private hospitals aggravated the health crisis in Lebanon. This makes it difficult for hospitals to pay their staff and purchase medical supplies. In addition, the shortage of dollars restricted the import of medicines and medical products, and they were lost in the market.
Private health care has become expensive for many as the economy has weakened and poverty levels have increased, putting further pressure on an already overloaded healthcare system.
Due to a shortage of anesthetic medications and most medical supplies, hospitals had resorted to limiting some laboratory tests and surgeries.
Jordan witnessed difficult months amid an economic downturn
Jordan’s government is taking steps to reduce restrictions considering the Corona pandemic. This positive step towards regaining normality in Jordan comes on the back of the government’s announcement that starting September 1, all exceptional measures imposed in response to the pandemic will be lifted.
The national Coronavirus vaccination program yielded promising results, with more than two and a half million taking one dose and about one and a half million acquiring two doses. At the same time, the percentage of infected people who tested positive dropped to less than 3 percent.
The case of controlling the spread of the Coronavirus came after Jordan witnessed difficult months, with over 10,000 infections recorded on some days, and the medical sector almost facing a health system failure, after hospitals and isolation rooms were overcrowded, and hospitals suffered from a shortage of medical products.
Jordan is experiencing its worst economic downturn in three decades, with the economic contraction rate reaching 1.6 percent, at a time when the country’s public debt exceeds $7 billion. Therefore, the government’s decisions to ease exceptional measures are not based on epidemiological trends but are also influenced by the country’s difficult economic situation. According to the Statistics Department, the unemployment rate hit 25 percent in Q1 2021 owing to its consequences and threat to societal peace.
The Jordanian government is forced to open the market. However, despite the World Bank’s testimony that the government’s fiscal stimulus packages have reduced the devastating effects over the last year, experts continue to raise warning bells: the budget deficit will exceed the $2 billion in 2021.
What needs to be done
The effectiveness of a public health system is not the function of only how well it manages a crisis. Its effectiveness also depends on poverty, unemployment, social justice, social empowerment, and good governance.
While the Arab countries’ response to the virus was focused on the immediate health effects, they ignored the response’s potential indirect and long-term results.
The pandemic exposed public health weaknesses in some Arab countries, such as a lack of resources, a dispersed workforce, and insufficient and weak infrastructures. Therefore, governments should enhance their investments in public health and preventive care. This may not always mean acquiring more financial resources. But they can invest a larger amount of their health budget in public health because the effects of the pandemic have begun to appear, especially in tourism, which accounts for up to 15 percent of Egypt’s GDP and 14percent in Jordan, 12 percent in Tunisia and 8 percent in Morocco.